Secretions of the small intestine, liver, gall bladder, and pancreas Flashcards
(80 cards)
Where does the majority of chemical digestion and absorption of nutrients, electrolytes and water take place in the GIT?
- small intestines
What are ther 3 parts of the small intestines called from top to bottom?
1 - duodenum
2 - jejunum
3 - ileum

What is the name of the spincter that facilitates movement from the stomach into the duodenum
- pyloric sphincter

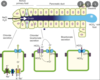
What are the 3 main secretions into the duodenum of the small intestines?
- intestinal juice (mucus/HCO3-)
- pancreatic juice (digestive enzymes)
- bile (fat emulsifier)
In addition to pancreatic juice, bile salts and intestinal juice, hormones can be secreted into the duodenum. What are the endocrine enzymes that are secreted that we need to know about?
- secretin
- cholecystokinin [CCK]
- glucose dependent insulinotrophic peptide [GIP]
The secretion of endrocrine secretions secretin, cholecystokinin [CCK] and glucose dependent insulinotrophic peptide [GIP] have an important functions in the duodenum. What 2 main secretions do they regulate in the duodenum?
- regulate bile and pancreatic secretions
Secretin is secreted by endocrine cells in the small intestines, which cells in the duodenum secrete it and what is the role of this hormone?
- peptide hormone secreted by S cells in duodenum
- regulates water homeostasis and pH
- regulates pH by secretions in the stomach, pancreas, and liver

Is secretin secreted into the lumen of the small intestines or into the blood stream?
- can be both
What is cholecystokinin and what is its main function?
- a peptide hormone
- secreted by enteroendocrine cells of te duodenum
- stimulates digestive enzymes and bile to be released
- can also act as a hunger supressant

What cells secrete glucose dependent insulinotrophic peptide (GIP) and what is the function for GIP?
- K cells in duodenum (hormone)
- trophic means to secrete and insulin tells you what
- inhibits gastric acid secretion
Cells at the tip of the microvilli are called enterocytes, what are they primarily involved in?
- absorption

What are goblet cells?
- cells in small intestines that secrete mucous

What are enteroendocrine cells?
- specialized cells found within the GIT stomach and pancreas
- able to secrete hormones when stimulated

Enteroendocrine cells are able to secrete hormones. They can secrete locally or systematicall, how do they do this and what are the different effects?
- local secretion = local messenger
- blood secretion = systemic effects
What are paneth cells that can be found in the epithelium of the small intestines?
- highly specialized secretory epithelial cells
- produce dense granules containing antimicrobial peptides and immunomodulating proteins
- main role immunotherpay

What are Brunners glands and where is the only place they can be found?
- glands are located in the submucosa of the duodenum

Brunners glands can only be found in the duodenum, what is their purpoose?
- secrete HCO3- and mucus
- increase pH and protect mucus
What cell in the walls of the GIT differentiate into different epithelial cells and drive shedding of epithelail cells?
- stem cells

Epithelial cells of the GIT have a high turnover, how often do they generally shed?
- 3-6 days
As the epithelial cells have a high regenerative capacity, what are they susceptible to in relation to a specific type of treatment?
- cancer treatment
- X-rays
- chemotherapy
Do paneth cells come from stem cells?
- no
- they come from daughter cells
- migrate downwards instead of upwards

What is intestinal juice, and what is it made up of?
- solution that facilitates digestion in the small intestines
- enterocytes secrete water containing electrolytes
- paneth cells secrete lysozyme to degrade bacteria
- goblet cells secrete mucus
- brunners glands secrete alkaline mucus
What is the main role of bile in the small intestines?
- fat emulsification
What is pancreatic juice?
- composed of digestive enzymes and bicarbonate
- eznymes are screted by acinar cells in pancrease
- bicarbonate is secreted from the epithelial cells lining small pancreatic ducts