03-07 Absorption Physio; Malabsorptive D/O Flashcards
• To be able to recall/describe normal digestion and absorption of fats, carbohydrates, proteins and vitamins • Describe/define the different pathophysiologic defects causing maldigestion and malabsorption involving the following: intraluminal digestion, intraluminal transfer to mucosa, mucosal digestion, mucosal processing, mucosal export • Describe the clinical manifestations and pathophysiologic mechanisms of the following disorders. Outline how each disorder illustrates one of the ab
<p>Hartnup Dz 101</p>
<p>A.D. mutation in renal & GI neutral AA (<em>tryptophan, histidine, phenylalanine</em>) transport in both gut and kidneys</p>
<ul>
<li>Usually Hartnup is asymptomatic
<ul>
<li>depends on genetics/penetrance</li>
</ul>
</li>
<li>Can lead to pellagra b/c tryptophan is a neutral AA that is broken down into niacin in the liver
<ul>
<li>niacin deficiency leads to pellagra</li>
<li>Rarely: niacin def → cerebellar ataxia & psychosis</li>
</ul>
</li>
<li>Niacin deficiency rare b/c
<ul>
<li>other dietary sources</li>
<li>can still absorp Trp as part of an oligopeptide that cgets absorbed paracellularly</li>
</ul>
</li>
</ul>
<p>Cystinuria 101</p>
<p>Autosomal recessive defect in SC3A1 dibasic AA transporter in gut and kidney</p>
<ul>
<li>Cystine least soluble of dibasic AAs (cystine, ornithine, arginine, lysine)</li>
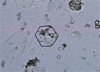
<li>precipitates in acid milieu of kidney→cystine kidney stones
<ul>
<li>see crystal here</li>
</ul>
</li>
</ul>
<p>Loss of enterohepatic circulation can cause deficiencies in?</p>
<p>Fat-soluble vitamins Vit A, D, E, K</p>

<p>coloretic diarrheais caused by</p>
<p>caused by bile salts irritating the colon</p>
<ul>
<li>can happen s/p T.I. resection</li>
</ul>
<p>Irritation of colon leads to increase extrusion of Cl- ions</p>
<ul>
<li>Na+ follows</li>
<li>H2O follows</li>
<li>diarrhea follows</li>
</ul>
<p>scalloped duodenal folds should make you think of</p>
<p>Celiac Dz</p>

<p>OBJECTIVE: describe normal digestion and absorption (including <u>where</u> it's absorbed) of carbs</p>

<p><strong>LOCATION OF CARB ABSORPTION</strong></p>
<ul>
<li>Very little in the duodenum</li>
<li>Most in jejunum</li>
<li>Less in distal small bowel</li>
<li>None in colon*
<ul>
<li>*2-20% of starches don't get absorbed→colon→ bacteria breakdown to SFACs (e.g.propionate, acetate, butyrate) + gas→ SCFAs absorbed by colonic enterocytes</li>
</ul>
</li>
</ul>
<p><strong>STEPS OF CARB DIGESTION AND ABSORPTION</strong></p>
<ol>
<li>Physical denaturation
<ul>
<li>mastication and antral grinding</li>
</ul>
</li>
<li>intraluminal digestion
<ul>
<li>starch--amylase--> oligosaccharides</li>
<li>both salivary (↓ effective b/c inactivated ↓ stomach pH) and pancreatic</li>
</ul>
</li>
<li>brush border digestion
<ul>
<li>di- & oligo-saccharides--b.b. disaccharidases—>monos</li>
<li>see image here</li>
</ul>
</li>
<li>transport (see image on reverse)</li>
</ol>
<ul>
<li><u>Apical membrane</u>: Two proteins
<ul>
<li>Fructose: Facilitated diffusion (GLUT5)</li>
<li>Gluc& Galactose: Active transport (Na/gluc transport - SGLT1)</li>
</ul>
</li>
<li><u>Basolateral membrane</u>: Single protein
<ul>
<li>Facilitated diffusion (GLUT2)</li>
</ul>
</li>
</ul>

<p>OBJECTIVE: describe normal digestion and absorption of protein</p>
<p><strong>Similar</strong> to carbs</p>
<ul>
<li>Major proteins hydrolyzed to oligopeptides and amino acids within the lumen</li>
</ul>
<p><strong>Unlike</strong>carbohydrates</p>
<ul>
<li>BOTH small polymers AND amino acids are absorbable</li>
<li>Proenzymes require conversion</li>
</ul>
<p><strong>STEPS OF DIGESTION AND ABSORPTION</strong></p>
<ol>
<li>Mechanical breakdown</li>
<li>Gastric hydrolysis
<ol>
<li>↓ gastric pH causes minimal protein hydrolysis</li>
<li>Gastric pepsinogen activated by acid to pepsin
<ul>
<li>Optimum pH ~2; inactivated by pancreatic juice</li>
<li>Partially digests 10-15% of dietary protein</li>
<li>NOT essential for protein digestion</li>
</ul>
</li>
</ol>
</li>
<li>Trypsin and luminal (premucosal) digestion
<ol>
<li>Pancreas releases trypsinogen
<ul>
<li>Activated by brush border enterokinase (and trypsin!)</li>
</ul>
</li>
<li>Trypsin
<ul>
<li>The key! activates 4 other peptidases</li>
<li>Quickly inactivates itself via autodigestion</li>
</ul>
</li>
<li>Brush border
<ul>
<li>Hydrolyzes larger peptides (3-8 AAs)</li>
</ul>
</li>
</ol>
</li>
<li>Absorption
<ol>
<li>Apical membrane AA transporters
<ul>
<li>Redundant: overlap for chemically similar AAs</li>
</ul>
</li>
<li>Di-, tri-, tetra- absorbed <strong>intact</strong> via carrier molecules
<ul>
<li><u>Cytosolic</u> peptidases then hydrolyze to AA’s</li>
</ul>
</li>
<li><u>Paracellular</u> route for <strong>intact</strong> peptides</li>
</ol>
</li>
</ol>

<p>OBJECTIVE: describe normal digestion and absorption of fats</p>
<ol>
<li><strong>Emulsified</strong> by the motion of chewing and antral grinding
<ul>
<li>provides more surface area for the lipases</li>
<li>bile salt stabilize this emulsion</li>
</ul>
</li>
<li>Fat —gastric/lingual <strong>lipases</strong>→ TALs & DALs
<ul>
<li>special acid and pepsin resistant lipase</li>
<li>inactivated once in duodenum by
<ul>
<li>neutral pH</li>
<li>trypsin digests it</li>
</ul>
</li>
</ul>
</li>
<li>CCK & GIP → ↑ biliary and <strong>pancreatic lipase</strong> secretions (bile salts, panc lipase)
<ul>
<li>TALs/DALs—panc.lipase→ MAG + 2FAs</li>
<li>panc lipase needs co-factors
<ul>
<li>neutral pH</li>
<li>co-lipase</li>
<li>bile salts</li>
</ul>
</li>
</ul>
</li>
<li>Micells form w/ bile salts & phospholipids → absorbed</li>
<li>Chylomicrons formed in enterocytes</li>
<li>Post-processing of dietary fat</li>
</ol>
<p>OBJECTIVE: describe normal digestion and absorption of vitamin B12</p>
<p>—Name one things that can go wrong at each step to cause B12 deficiency</p>
<p>see image here</p>
<ol>
<li>Decreased Intrinsic Factor secretion
<ul>
<li>Pernicious anemia, Gastrectomy</li>
</ul>
</li>
<li>Increased R factor B12 binding
<ul>
<li>Pancreatic insufficiency</li>
</ul>
</li>
<li>Increased bacterial B12 uptake
<ul>
<li>Bacterial overgrowth</li>
</ul>
</li>
<li>Decreased ileal B12 absorption
<ul>
<li>Crohn’s disease, ileal resection</li>
</ul>
</li>
</ol>

<p>OBJECTIVE: Describe/define the different pathophysiologic defects causing maldigestion and malabsorption involving the following steps in<strong>carbohydrate</strong> digestion and absorption: intraluminal digestion, intraluminal transfer to mucosa, mucosal digestion, mucosal processing, mucosal export</p>
<p>See image</p>

<p>OBJECTIVE: Describe/define the different pathophysiologic defects causing maldigestion and malabsorption involving the following steps in<strong>protein</strong> digestion and absorption: intraluminal digestion, intraluminal transfer to mucosa, mucosal digestion, mucosal processing, mucosal export</p>
<p>See image</p>

<p>OBJECTIVE: Describe/define the different pathophysiologic defects causing maldigestion and malabsorption involving the following steps in <strong>fat</strong> digestion and absorption: intraluminal digestion, intraluminal transfer to mucosa, mucosal digestion, mucosal processing, mucosal export</p>
<p>See image</p>

<p>OBJECTIVE: Describe/define the different pathophysiologic defects causing maldigestion and malabsorption involving the following steps in<strong>fat</strong> <u>absorption</u>(only).</p>
<p>see image</p>

<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of lactase deficiency.</p>
<ul>
<li>bloating, pain, gas, diarrhea that improves w/ fasting</li>
</ul>
<p>PATHOPHYSIOLOGY</p>
<ul>
<li>lactase activity is lower:
<ul>
<li>with age</li>
<li>in non-Northern Europeans</li>
<li>sometimes after infections or inflammation</li>
</ul>
</li>
<li>lactose in the gut:
<ul>
<li>acts as osmotic laxative</li>
<li>is fermented into:
<ul>
<li>SCFAs → omsotic lax</li>
<li>H2, methane → farts</li>
</ul>
</li>
</ul>
</li>
</ul>
<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of pancreatic insufficiency.</p>
<p><strong>CLINICAL MANIFESTATIONS</strong></p>
<ul>
<li>steatorrhea</li>
<li>fat soluble vitamin malabsorption</li>
<li>frequently, insulin dependent diabetes</li>
<li>Other well known sequelae:
<ul>
<li>metabolic bone disease</li>
<li>B12 deficiency</li>
<li>oxalate kidney stones</li>
</ul>
</li>
</ul>
<p><strong>PATHOPHYSIOLOGY</strong></p>
<p><u>Carb Malabsorption</u></p>
<ul>
<li>Amylase production</li>
<li>Bicarbonate (optimal pH) and Cl- for amylase</li>
</ul>
<p><u>Protein Malabsorption</u></p>
<ul>
<li>Pancreatic proteases (zymogens and active)</li>
</ul>
<p><u>Fat Malabsorption</u></p>
<ul>
<li>↓ Bicarbonate (optimal pH)</li>
<li>↓ Lipase, colipase</li>
<li>steatorrhea → ↑ oxalate absorption by fat binding Ca/Mg (saponification) → not enough Ca/Mg to bind and prevent oxalate absorption</li>
</ul>
<p><u>Vitamin/Mineral Malabsorption</u></p>
<ul>
<li><span>B12 (cobalamin) Deficiency</span>
<ul>
<li><span>Insufficient pancreatic proteases to digest dietary R factors that bind cobalamin</span></li>
</ul>
</li>
<li><span>Metabolic bone disease</span>
<ul>
<li><span>Vit D deficiency (along w/ A, D, & E)</span></li>
</ul>
</li>
</ul>
<p>Refer to notes “Pancreatic Function/Disorders of the Exocrine Pancreas" for pathophysiology.</p>
<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of Bile salt deficiency.</p>
<p>CLINICAL MANIFESTATIONS</p>
<ul>
<li>steatorrhea</li>
<li>Deficiency of Vitamins A, D, E and/or K</li>
</ul>
<p>PATHOPHYSIOLOGY</p>
<ul>
<li> Often caused by resection of the terminal ileum where 95% of bile salts are reabsorbed</li>
<li>leads to inability to form micelles</li>
</ul>
<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of celiac disease.</p>
<p>CLINICAL MANIFESTATIONS</p>
<ul>
<li>"panmalabsorption"</li>
<li>iron deficiency anemia (b/c of )</li>
<li>unintended weight loss</li>
<li>diarrhea</li>
</ul>
<p>PATHOPHYSIOLOGY</p>
<ul>
<li>allergic rxn to gliadin within epithelium and subepithelium of the proximal small bowel</li>
<li>•HLA-DQ2 OR HLA-DQ8 genotype required
<ul>
<li>but not sufficient</li>
</ul>
</li>
<li>Fe-def happens because theduodenum (the site where divalent ions are absorbed) is affected</li>
<li>weight loss because the villi of the small bowel are eroded decreasing the surface area for absorption
<ul>
<li>see histo image here</li>
</ul>
</li>
<li>diarrhea b/c:
<ul>
<li>destroys neuroendocrine cells→ impairs CCK/Secretin release → decreased pancreaticobiliary secretion and steatorrhea</li>
<li>↓ brush border hydrolases, peptidases, transport proteins → CHO and protein malabsorption</li>
<li>↓ villous structure → ↓ surface area</li>
<li>↑ inflam mediators → ↑intestinal secretion</li>
</ul>
</li>
</ul>

<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of small bowel bacterial overgrowth.</p>
<p>CLINICAL MANIFESTATIONS</p>
<ul>
<li>steatorrhea</li>
<li>sx of ADEK absorption</li>
<li>B12 (cobalamin) deficiency sx
<ul>
<li>megaloblastic anemia (could also be 2° to folate def)
<ul>
<li>hypersegmented neutrophils</li>
</ul>
</li>
<li>neuro ∆s (<u>not</u> caused by low folate)</li>
<li>atrophic glossitis, etc.</li>
</ul>
</li>
</ul>
<p>PATHOPHYSIOLOGY</p>
<ul>
<li>bacteria dis-conjugate bile salts → makes them absorbable so quickly they can't work → fat malabsorption → A, D, E, K and steatorrhea</li>
<li>Bacteria can also bind B12</li>
</ul>
<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of abetalipoproteinemia.</p>
<p><strong>CLINICAL MANIFESTATIONS</strong></p>
<ul>
<li>infancy fat malaborption</li>
<li>low VLDL</li>
<li>Vit ADEK deficiencies</li>
</ul>
<p><strong>PATHOPHYSIOLOGY</strong></p>
<ul>
<li>inherited mutation in microscopmal triglyceride transfer proteins</li>
<li>apo B-48 and B-100 deficiencies → No ApoB48 to form <u>chylomircrons</u></li>
</ul>
<p>OBJECTIVE: Describe the clinical manifestations and pathophysiologic mechanisms of Whipple's disease.</p>
<p><strong>CLINICAL MANIFESTATIONS</strong></p>
<ul>
<li>Fat malabsorption
<ul>
<li>Fatty acid diarrhea</li>
</ul>
</li>
<li>Protein losing enteropathy
<ul>
<li>Edema, ascites, pleural effusion</li>
<li>Lymphopenia-susceptible to infection</li>
</ul>
</li>
</ul>
<p><strong>PATHOPHYSIOLOGY</strong></p>
<p><em>T. whipplei</em> infection</p>
<p>may be acquired from exposure to dust borne soil in individuals with impaired cellular immunity</p>
<p>Bacteria grow within “foamy” macrophages in lamina propria, mesentery and lymph nodes → enlarge → lymphangiectasia</p>
<p> </p>
<p>OBJECTIVE: List the signs and symptoms of maldigestion and malabsorption of major nutrients and vitamins</p>
<p>.bleck</p>
<p>OBJECTIVE: define diarrhea</p>
<p>Fluid secretion and/or failure to absorb water and electrolytes</p>
<p>OBJECTIVE: define maldigestion</p>
<p>Failure to break down complex nutrients</p>
<p>OBJECTIVE: define malabsorption</p>
<p>Failure to absorb products of digestion</p>
<p>These are serum glucose and H2 breath test results from a lactose challenge test in a normal individual.</p>
<ul>
<li>How would these results look in someone w/ lactase deficiency?</li>
</ul>


<p><strong>Bacterial overgrowth</strong></p>
<ul>
<li>predisposing factors</li>
<li>presentation</li>
<li>Diagnosis</li>
<li>pathophys</li>
</ul>
<p>PREDIPOSING FACTORS</p>
<ol>
<li>Anatomic derangements
<ul>
<li>Ileocecal resection, fistula</li>
</ul>
</li>
<li>Achlorhydria
<ul>
<li>H+ is an antibiotic that ↓ bacterial flora</li>
</ul>
</li>
<li>Stasis
<ul>
<li>Impaired motility and aging, impaired MMC’s (migrating motor complexes)</li>
</ul>
</li>
</ol>
<p><strong>PRESENTATION</strong></p>
<ul>
<li>most pts: nonspecific sx of bloating, flatulence, or abd discomfort, or asymptomatic</li>
<li>Many pts w/ severe have diarrhea or steatorrhea</li>
<li>Rarely wt loss due to severe diarrhea, malabsorption, or poor oral intake</li>
</ul>
<p><strong>DIAGNOSIS</strong></p>
<ul>
<li>Quantitative small bowel culture</li>
<li>(+) Breath test for H2, methane production after eating carbs</li>
</ul>
<p><strong>PATHOPHYS</strong></p>
<ul>
<li>> 106 aerobes/anaerobes per ml → deconjugation of bile salts → fat malabsorption
<ul>
<li>Deconjugated bile salts, unionized at duodenal pH, do not form micells</li>
</ul>
</li>
<li>Make SCFAs →H2, CO2, and methane</li>
<li>Bacterial toxins damage mucosa</li>
<li>•Bacterial bind B12 (cobalamin)
<ul>
<li>Megaloblastic anemia, and all the rest</li>
</ul>
</li>
</ul>



