Skin/Fat/Cartilage Grafts Flashcards
A 55-year-old woman undergoes composite resection of the right mandibular body and floor of the mouth. Closure with a fibular free flap is performed. A photograph is shown. Which of the following mechanisms best describes the healing process associated with vascularized bone transfers?
A) Endochondral ossification
B) Osteochondrosis
C) Osteoconduction
D) Osteogenesis
E) Osteoinduction

The correct response is Option D.
Osteogenesis is the formation of new bone by cells in a flap/graft that survive the transfer. This is the primary mechanism by which a vascularized bone graft heals. The pedicle keeps the bone alive so that primary bone healing can occur between the graft and recipient site. Osteoblasts from both locations participate in the formation of new bone at the interface between graft and native bone. Advantages of a vascularized bone graft include the ability to place the graft into a hostile environment such as an irradiated wound bed and immediate structural support with shortened time to bony union compared with nonvascularized cortical grafts.
Osteoinduction refers to the direct stimulation of mesenchymal cells at the recipient site by bone morphogenetic protein to differentiate into osteoprogenitor cells. This mechanism of action is associated with the healing of cancellous bone grafts and demineralized bone matrix.
Endochondral ossification is the process by which the cartilaginous soft callus covering a fracture is transformed into bone.
Osteochondrosis refers to a family of ossification disorders in children.
Osteoconduction (creeping substitution) is the primary method by which cortical bone grafts heal. During osteoconduction, cells and blood vessels from the recipient bed grow into the graft. The bone graft becomes a template for the deposition of new bone and the graft resorbs. Neovascularization is complete by 6 to 8 weeks, but ultimate strength of cortical grafts is not seen until 6 to 12 months, at which time the graft is comparable to a vascularized bone graft.
2018
A 55-year-old woman is scheduled to undergo autologous fat grafting to improve the upper inner quadrant aesthetic contour of the breasts. Six months ago, she underwent bilateral mastectomy and breast reconstruction with deep inferior epigastric perforator flap coverage. The patient does not have or desire breast implants. Which of the following percentage ranges most accurately describes the likelihood of fat graft survival in this patient?
A) 10%
B) 35%
C) 60%
D) 85%
The correct response is Option C.
Because of demonstration of the safety, efficacy, and improvements in the harvest and preparation of fat, autologous fat grafting or liposculpting is gaining popularity to adjust aesthetic breast contour irregularities after all forms of breast reconstruction. The most common complication of fat injection remains the resorption of the grafted fat.
Fat graft volume retention has been studied previously. Employing radiologic volumetric data analysis in fat grafting for cosmetic and reconstructive breast surgery demonstrates volume retention between 50 to 80% and this retention may be time and volume dependent.
Resorption of grafted fat may be attributable to apoptosis, a reduction in adipocyte volume after transplantation and survival, or a reduction in the fluid content of the grafted mixture.
2018
A 34-year-old man sustains deep second-degree burns to the forearm. He is brought to a local burn center. A skin graft is chosen as the coverage method. Which of the following management techniques offers the highest likelihood of skin graft survival in this patient?
A) Complete fascial excision
B) Early range of motion
C) Keeping the graft uncovered postoperatively
D) Placing a full-thickness graft
E) Placing a meshed graft
The correct response is Option E.
The principles of burn wound skin grafting dictate that first, a clean wound must be obtained. This is achieved through operative debridement and washout, to remove all necrotic eschar, and eliminate any possible source of bacteria or infection.
In most cases of second-degree burns, a complete fascial excision is not necessary, as this proceeds much deeper than the affected tissue. Instead, a tangential excision is used to remove burn eschar, in layers, until the necrotic tissue has been excised, and viable tissue remains at the base of the wound.
Following this, a split-thickness skin graft allows for greatest potential of graft survival. The use of a full-thickness graft will result in lower graft survival rates.
Meshing the skin graft prior to placement will improve survival, as it prevents accumulation of fluid or blood under the skin graft. Any collection of seroma or hematoma under the graft will prevent successful outcomes.
Placement of either a bolster dressing or a negative pressure (vacuum-assisted closure) dressing on the skin graft, will prevent mechanical shear forces, and improve graft survival rates. Thus, for the first 5 days after graft placement, any early motion or lack of dressing will result in greater risk of shear forces, and lower graft survival rates.
2018
A 52-year-old woman undergoes fat grafting of the upper right breast area to correct a contour indentation after implant reconstruction. Which of the following factors will most likely increase the success of fat grafting?
A) Abdominal donor site
B) Grafting soon after harvest
C) Rinsing the fat with Ringer’s lactate
D) Ultrasonic liposuction aspiration
E) Use of centrifuged fat
The correct response is Option B.
There is evidence that the longer fat is exposed at room temperature, the lower the adipocyte viability. There may be complete loss of stem cell viability by 4 hours at room temperature and 24 hours at 4°C (39°F).
There is no high-level evidence suggesting that centrifuging or rinsing fat increases viability. There is also no evidence for enhanced fat survival based on donor site, such as the abdomen, thigh, or arm. Use of local anesthesia does not appear to hinder graft survival. It does appear that less mechanical trauma with low-shear harvesting instruments is helpful. Ultrasonic liposuction is designed to rupture fat cells and would likely hinder graft survival.
Fat grafting is an increasingly common tool, although results appear to be operator-dependent based on wide ranges of success in published reports. There is no absolute agreed-upon method of measuring fat survival. Most studies use volumetric analysis with imaging. More future long-term studies are needed. At this time it appears that the commonality of successful results is delicate handling of the fat.
2018
A 43-year-old man undergoes wound closure with a split-thickness skin graft harvested from the left thigh. Which of the following skin appendages are the primary source of multipotent stem cells responsible for reepithelialization of the donor site?
A) Apocrine glands
B) Arrector pili
C) Eccrine glands
D) Hair follicles
E) Sebaceous glands
The correct response is Option D.
Hair follicles contain multipotent stem cells that are activated upon the start of a new hair cycle and upon wounding to provide cells for hair follicle and epidermal regeneration. In the hair follicle, stem cells reside in the bulge area. Bulge cells are relatively quiescent compared with other cells within the follicle but can be recruited during wound healing to support reepithelialization. Sebaceous, apocrine, and eccrine glands secrete fluids that are involved in lubricating, coating, or cooling the skin. Arrector pili are responsible for motility of cutaneous hair in response to tactile stimulation or low temperatures.
2018
A 23-year-old man comes to the office for post-traumatic cranial reconstruction 6 months after a motor vehicle collision. Physical examination shows a 5 × 4-cm full-thickness calvarial defect in the left parietal region. A titanium/hydroxyapatite cement cranioplasty reconstruction is planned. Which of the following mechanisms best describes the healing process associated with hydroxyapatite?
A) Endochondral ossification
B) Osteochondrosis
C) Osteoconduction
D) Osteogenesis
E) Osteoinduction
The correct response is Option C.
Restoration of craniofacial contour after infection, tumor resection, or trauma can be quite challenging. Autologous bone grafts have long been considered the gold standard because of their high likelihood of osseointegration/healing, and low risk of rejection or infection. Autologous bone grafts, however, have several drawbacks including unpredictable resorption, donor site morbidity, limited availability, prolonged operative times, and difficulty to contour. As a result, there has been an ongoing search for alternative means of reconstruction with alloplastic material.
The ideal bone substitute should be chemically inert, easily contoured, able to retain a stable shape over time, strong, resistant to infection or foreign body reaction, inexpensive, and capable of osseointegration and tissue ingrowth. Methylmethacrylate has been used frequently for calvarial reconstruction but suffers several drawbacks, including infection requiring removal of implant, plate fracture, lack of osseointegration, difficulty shaping after polymerization, and necrosis of surrounding tissue due to the exothermic nature of the curing process.
Among the most promising and well-tolerated alloplastic materials for craniofacial skeletal reconstruction are the calcium phosphate–based compounds. Hydroxyapatite [Ca(PO4)6(OH)2] forms the principal mineral component of bone and constitutes 60% of the calcified human skeleton. Calcium phosphate compounds are bioactive and capable of osteoconduction and osseointegration.
Osseointegration refers to the direct chemical bonding of an alloplast to the bony surface without an intervening fibrous tissue layer. During osteoconduction (creeping substitution), the alloplast acts as a nonviable scaffold for ingrowth of blood vessels and osteoprogenitor cells from the recipient site. Subsequently, the graft/alloplast is resorbed and replaced with new bone. This mechanism is also associated with the healing of cortical bone grafts.
Hydroxyapatite (HA) cement is a mixture of tetracalcium phosphate and dicalcium phosphate anhydrous, which react in an aqueous environment to form a paste that can be easily applied and sculpted to fit the surgical defect. HA cement sets isothermically, so there is no risk of thermal damage to the surrounding tissues. Additional benefits of HA include “off the shelf” ease of use, maintenance of volume over time, lack of radiologic scatter, and low incidence of infection.
Osteoinduction refers to the direct stimulation of mesenchymal cells at the recipient site by bone morphogenetic protein to differentiate into osteoprogenitor cells. This mechanism of action is associated with the healing of cancellous bone grafts and demineralized bone matrix. Endochondral ossification is the process by which the cartilaginous soft callus covering a fracture is transformed into bone. Osteogenesis is the process by which vascularized bone grafts heal. Viable osteocytes survive the transplantation process and produce new bone at the recipient site. Osteochondrosis refers to a family of ossification disorders in children.
2017
A 46-year-old man with type 1 diabetes mellitus is evaluated for an infected foot ulcer. After adequate surgical debridement, a collagen bilayer matrix is used for coverage. Which of the following clinical factors represents the greatest risk for failure of reconstruction?
A) Anatomic location
B) Exposed bone
C) Exposed tendon
D) Polymicrobial infection
E) Type 1 diabetes mellitus
The correct response is Option D.
Collagen bilayer matrices have become an important option in the reconstructive ladder for lower extremity wounds. Studies have demonstrated the ability of these dermal regeneration templates to neovascularize and heal into pliable, durable coverage in an attempt to achieve stable wound healing and maintain limb length. Many of these studies were performed in the setting of diabetic wounds with exposed bone or tendon, thus each of these settings does not represent a contraindication. Adequate debridement, including clearance of any polymicrobial infection, is one of the keys to successful reconstruction.
2017
A 47-year-old man undergoes split-thickness autografting for the treatment of a forearm burn. Which of the following donor site dressings is most appropriate to optimize wound healing?
A) Alginate covered with occlusive dressing for 7 days
B) Moist gauze covered with occlusive dressing for 7 days
C) Petrolatum gauze covered with occlusive dressing for 2 days, then left open to air
D) Petrolatum gauze left open to air
E) Xenograft left open to air
The correct response is Option A.
To optimize wound healing, a moist wound-healing environment has been shown to be superior to a dry wound-healing environment. Studies on split-thickness skin graft donor sites have not been very well designed, but many studies suggest that a moist dressing is better than a dry dressing, and several review papers support this concept. Although leaving petrolatum gauze open to air is very common and may be the most practical option in certain circumstances, it does not optimize wound healing compared with a moist dressing. The only options listed that provide a moist environment for the duration required for early reepithelialization are gauze covered with occlusive dressing and alginate dressings. Gauze covered with occlusive dressing would not work well, because conventional gauze would stick to the wound and be very difficult to remove without causing significant tissue injury. Alginate dressings are emerging as an excellent option for split-thickness skin graft donor site wounds. They are adaptable, absorptive, nonadhesive, antibacterial, and provide a moist environment for wound healing.
2017
Which of the following best describes the immediate mechanism of skin graft survival following placement onto the recipient wound bed?
A) Dermal contraction
B) Encapsulation
C) Inosculation
D) Revascularization
E) Serum imbibition
The correct response is Option E.
Serum imbibition describes the earliest stage of skin graft healing. Immediately after placement onto the wound, the graft becomes edematous and may increase its mass up to 30 to 40%. Plasma leaks from recipient bed capillaries and venules and fills the space between the wound bed and the graft. Fibrinogen within the plasma settles out and forms a fibrin bond, which helps anchor the graft to the wound. The graft passively absorbs nutrients from the underlying serum by diffusion during the first 48 hours. Metabolism within the graft becomes anaerobic and the pH level falls to 6.8. The metabolic demands of the graft also fall, with ATP levels falling 70% and glucose levels falling 80%.
Revascularization and inosculation describe the second stage of skin graft healing. These processes began shortly after graft placement, but it takes approximately 4 to 5 days for the graft to become vascularized, with maximal flow developing by day 29. Revascularization refers to direct ingrowth of new blood vessels into the graft from the underlying wound bed. Inosculation describes a process by which blood vessels from the underlying wound bed connect with existing vessels in the skin graft. More recent evidence suggests that both of these processes play a role in the development of vascularization within the skin graft: existing vasculature within the skin graft undergoes some level of degeneration. However, the acellular basal lamina persists and provides a conduit for the ingrowth of a new vascular tree from the host wound bed.
Primary contraction of a skin graft occurs immediately after harvest and is due to the recoil of elastic fibers within the dermis. Grafts with a larger amount of included dermis (e.g., full-thickness grafts) have greater primary contraction. Secondary contraction refers to contraction after the wound heals. This process is mediated by myofibroblasts and occurs more frequently in grafts with a thinner dermal component (e.g., split-thickness grafts). A larger dermal component appears to suppress proliferation of myofibroblasts within the wound. Encapsulation refers to the development of a fibrous scar capsule around a foreign device such as a breast implant.
2017
A 65-year-old man comes to the office because of a 6 × 8-cm open wound on the forearm. The wound currently has healthy granulation tissue and does not appear infected. Which of the following is an advantage of split-thickness skin grafting over full-thickness skin grafting in this patient?
A) Less metabolic demand required from wound bed
B) Less secondary contraction from elastin fibers
C) More primary contraction from myofibroblasts
D) Occurrence of inosculation before plasmatic imbibition
E) Presence of intact skin appendages within graft
The correct response is Option A.
Split-thickness skin grafts require less metabolic demand from the wound bed compared with full-thickness skin grafts. In situations where the wound bed may not supply adequate nutrient diffusion through the graft, a full-thickness graft may develop superficial epidermolysis.
Skin graft viability is initially based on plasmatic imbibition from the serous exudate of the wound, followed by inosculation and angiogenesis. After graft take, remodeling and scar maturation occur. Primary contracture of a graft is from elastin fibers in the dermis, whereas secondary contracture is from myofibroblast activity.
Split-thickness grafts contain epidermis and a variable amount of dermis compared with full-thickness grafts, which, by definition, contain both epidermis and the entire dermal layer. Full-thickness grafts contain intact skin appendages, whereas split-thickness grafts do not; this allows the donor site for split-thickness grafts to reepithelialize. Split-thickness grafts therefore undergo less primary and more secondary contraction.
2016
A 9-year-old boy with unilateral cleft lip and palate undergoes alveolar bone grafting with a cancellous iliac bone graft. Which of the following best describes the mechanism of bone healing?
A) Endochondral ossification
B) Osteochondrosis
C) Osteoconduction
D) Osteogenesis
E) Osteoinduction
The correct response is Option E.
Osteoinduction refers to the direct stimulation of mesenchymal cells at the recipient site by bone morphogenetic protein to differentiate into osteoprogenitor cells. This mechanism of action is associated with the healing of cancellous bone grafts and demineralized bone matrix.
Osteoconduction (creeping substitution) is the primary method by which cortical bone grafts heal. During osteoconduction, cells and blood vessels from the recipient bed grow into the graft. The bone graft becomes a template for the deposition of new bone and the graft resorbs. Neovascularization is complete by 6 to 8 weeks, but ultimate strength of cortical grafts is not seen until 6 to 12 months, at which time the graft is comparable to a vascularized bone graft.
Osteogenesis is the formation of new bone by cells in a flap/graft that survive the transfer. This is the primary mechanism by which a vascularized bone graft heals. The pedicle keeps the bone alive so that primary bone healing can occur between the graft and recipient site. Osteoblasts from both locations participate in the formation of new bone at the interface between graft and native bone. Advantages of a vascularized bone graft include the ability to place the graft into a hostile environment such as an irradiated wound bed and immediate structural support with shortened time to bony union compared with nonvascularized cortical grafts.
Osteochondrosis refers to a family of ossification disorders in children. Endochondral ossification is the process by which the cartilaginous soft callus covering a fracture is transformed into bone.
2016
A 64-year-old woman is evaluated because of the aged appearance of the dorsal surfaces of the hands. Physical examination of the hands shows lipodystrophy. Autologous fat grafting is planned to improve the cosmetic appearance. Which of the following maneuvers is most likely to decrease the risk of fat necrosis and improve fat graft viability?
A) Placement of fat grafts in small aliquots
B) Postoperative prevention of pressure on grafted regions
C) Preparation of fat grafts with centrifugation
D) Use of ultrasound-assisted liposuction for fat graft harvest
The correct response is Option A.
The results of fat grafting are dependent upon the surgeon’s experience and technique. Strategies to increase the take of the fat graft and decrease fat necrosis include atraumatic harvest techniques. Placement of the graft in multiple small aliquots increases the availability for vascularity, and creating a lattice-like framework when depositing the grafts avoids large-volume deposits. Placement of the grafts in a few large-volume deposits is avoided to minimize fat necrosis and creation of fatty oil cysts. Centrifugation has mixed results in fat grafting.
2016
A 22-year-old woman is evaluated in the emergency department because of necrotizing fasciitis of the right upper extremity. BMI is 35 kg/m2. After adequate debridement, the entire extensor and flexor compartments are open with exposed tendon. A photograph is shown. Which of the following is the most appropriate initial method of reconstruction?
A) Anterolateral thigh free flap
B) Bilaminate neodermis
C) Full-thickness skin grafts
D) Pedicled abdominal flap
E) Split-thickness skin grafts
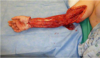
The correct response is Option B.
Although a bilaminate neodermis (Integra) artificial skin substitute has been traditionally used in the acute management of burns, there have been many successful reports incorporating its use in general reconstructive plastic surgery. Integra is a bioengineered dermal substitute consisting of a bilayer membrane system. The dermal replacement layer is composed of a cross-linked bovine tendon collagen-glycosaminoglycan (chondroitin-6-sulfate) matrix coated on one side with a synthetic polysiloxane polymer (silicone) layer. This layer functions as an epidermis to control moisture loss from the wound. The collagen matrix serves as a scaffold for ingrowth of fibroblasts, macrophages, lymphocytes, and capillaries and is ultimately replaced by host tissue. Integra “take” mirrors skin graft “take” and follows the sequence of 1) imbibition, 2) fibroblast migration, 3) neovascularization, and 4) maturation.
As the host tissue infiltrates the dermal layer, the collagen layer is biointegrated with the wound to form a vascular neodermis capable of accepting a split-thickness skin graft after a period of approximately 4 weeks. Proper patient selection and careful monitoring for infection or hematoma accumulation are crucial in this time period. After approximately 4 weeks, the silicone layer is removed and a thin (0.008- to 0.010-inch) skin graft can be applied.
Advantages of Integra use include improved cosmesis, diminished scar contracture or development of hypertrophic scar, off-the-shelf availability in large quantities, increased elasticity, and the ability to use thinner skin grafts with subsequent improvement in donor-site morbidity, scar, and time to heal. Other cited advantages include commensurate growth of the grafted tissue in children, potential avoidance of a microsurgical procedure, and placement over tendons with no significant reduction in tendon mobility. The disadvantages of Integra include its high cost, steep learning curve, need for at least two stages with subsequent increased time to final closure, potential for infection under the silicone layer, and lack of adnexal structures with patient concerns of skin dryness.
In this patient, use of Integra with delayed thin split-thickness skin grafts at 4 weeks will give the best outcome in terms of cosmesis and function. A photograph is shown. Split-thickness skin grafts are not a good option in this location because of the risk of graft loss with tendon exposure due to lack of viable paratenon and the risk of secondary contracture at the wrist and elbow. Full-thickness skin grafts would diminish the risk of secondary contracture but harvesting enough tissue to cover the entire arm would be impossible using the inguinal region as a donor site. Full-thickness grafts also require a healthier wound bed for optimal graft “take” and are not likely to heal over exposed tendons.
Free tissue transfer is an excellent technique for resurfacing the forearm, but in this patient, the thigh donor site would be difficult secondary to tissue thickness and the need for an extremely large flap. A better choice could be the scapular or parascapular donor site, perhaps in combination with a preliminary tissue expansion of that location. Obtaining enough tissue would be difficult. Banking the forearm in the abdomen would be less desirable as well, given her obesity and the need for a large surface area.
2016

A 30-year-old man requires bone grafting for repair of a severe nasal deformity after a bicycle collision. Which of the following is the optimal rib donor site for ease of exposure and limited morbidity?
A) First
B) Third
C) Fourth
D) Seventh
E) Eleventh
The correct response is Option D.
Ribs five through seven are commonly described as the ideal sites for harvesting because of ease of access and ample bone material compared with the more cephalic or caudal ribs. The seventh rib has the added advantage of being situated over the abdominal cavity, reducing the risk for pneumothorax during harvest. Ribs five and six are also suitable, and may hide better in the inframammary crease of women.
Ribs may be harvested either whole or split depending on the amount of material needed. If a whole-rib graft is required, as long as multiple adjacent ribs are not removed, morbidity is limited. Split-rib harvest offers the advantage of eventual bone regrowth, and the area can be harvested for bone grafting again in the future if needed. The eleventh rib provides a wide expanse of medial cartilage for harvest, although it is not an ideal bone donor site.
Rib grafts offer both cortical and cancellous bone material. The cortical bone is rigid and provides immediate structural support, though final incorporation and strengthening occur over many months. A well-vascularized wound bed is required for bone healing and incorporation. A split-rib inset provides the cancellous bone surface, which is more rapidly revasculuarized. If an entire bone is needed for grafting, then a vascularized bone graft or flap with microvascular anastomosis would be better suited.
2016
A 25-year-old woman is scheduled for correction of a deformity of the nasal dorsum caused by previous nasal trauma as a child. Autologous rib cartilage grafting of the dorsum is planned to correct the deformity. Which of the following complications is most likely in this patient?
A) Extrusion
B) Necrosis
C) Ossification
D) Resorption
E) Warping
The correct response is Option E.
The most consistent complication of cartilage grafting is the propensity to change shape or warp over time. This may be due to the presence of perichondrium or the nonuniform composition of the matrix that can affect the shape when it is placed.
Pure cartilage grafts tend to maintain shape, but grafts with an intact perichondrial layer can curl significantly and lead to unpredictable results. During septal graft harvest, care must be taken to elevate mucoperichondrial flaps in the proper plane. Likewise, auricular or costal cartilage grafts must be harvested in a subperichondrial plane. Removal of the perichondrium and softer outer cartilage layer leaves the more rigid cartilage core, which maintains shape more predictably.
Extrusion, necrosis, ossification, and resorption are not known to be affected by the presence or absence of the perichondrial layer. Fresh autologous grafts easily survive transplantation procedures and do not appear to resorb over time.
Autologous cartilage from septum, concha, or rib is considered the ideal graft material. These grafts have very low risk for infection or extrusion compared with an allograft. Cartilage grafts are tolerated well by nasal tissue.
2016
A 58-year-old man is referred by an orthopedic surgeon after undergoing open reduction and internal fixation of a fracture of the ankle after falling down stairs. The repair is complicated by wound dehiscence with 2 × 2 cm of exposed tibialis anterior tendon without paratenon. A photograph is shown. After debridement of healthy tissue, reconstruction is performed using bilaminate neodermis with placement of a standard bolster dressing. At which of the following times relative to placement of the bilaminate neodermis should split-thickness skin grafting be performed?
A) At the same time
B) 1 week after
C) 2 weeks after
D) 4 weeks after
E) 6 weeks after
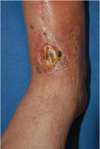
The correct response is Option D.
Integra is a bilaminate neodermal material that consists of an outer silicone sheet and an inner layer of bovine collagen and glycosaminoglycan (derived from shark cartilage), which acts as a scaffold for regeneration. Specifically, there is migration of host fibroblasts into the matrix, which subsequently proliferate and form collagen. Additionally, there is migration of endothelial cells that form a vascular network within the neodermis, which can subsequently act as a foundation to support staged split-thickness skin grafting, at which time the silicone outer layer is removed and a thin (usually 6–8/1000”) split-thickness autograft is applied. The success, or “take,” of the skin graft depends on whether the neodermis is vascularized sufficiently to maintain graft viability. A 2001 study by Moiemen et al. demonstrated clinically and histologically that this process takes 4 weeks on average, without the use of topical negative pressure.
A follow-up article from 2004 suggests this process can be accelerated from 4 weeks to an average of 7.25 days if topical negative pressure is used. Further follow-up studies based on the clinical appearance of the bilaminate neodermal matrix have suggested reduction in complication rates, improved patient tolerance, and enhanced and accelerated neovascularization with the use of topical negative pressure wound therapy. However, a study published in 2010 looking histologically at various time points could not demonstrate that topical negative pressure wound therapy accelerates neovascularization as verified by the presence of histologically patent vascular channels. The authors found that the median percentage of the template depth that demonstrated canalized channels was 0%, 20%, 61%, and 80% for days 7, 14, 21, and 28, respectively.
Because this question pertains to the use of bilaminate neodermal matrix with the use of a standard bolster dressing and not negative pressure wound therapy, most existing evidence indicates that the most appropriate timing is 4 weeks after placement of the bilaminate neodermis.
2016

A 30-year-old man who works as a laborer comes to the emergency department after sustaining avulsion injuries over the dorsum of the index, long, and ring fingers of his right dominant hand after being caught in a press. The wounds measure 3 × 1 cm each. Physical examination shows exposed extensor tendons from the proximal interphalangeal joint to the dorsal fold. Artificial dermis was placed. Which of the following is the most appropriate method of reconstruction?
A) Full-thickness skin graft
B) Radial artery free flap
C) Reverse radial forearm flap
D) Split-thickness skin graft
E) No further treatment
The correct response is Option D.
Split-thickness and full-thickness skin grafting directly over extensor tendons will lead to scarring due to lack of paratenon. Paratenon is necessary for tendon gliding. The use of artificial dermis can allow for tendon gliding. Artificial dermis has been shown to result in favorable aesthetic and functional outcomes. Although a second surgery is required, it results with lower donor site morbidity. Once the dermal template is adherent, it can then be grafted. The correct response is split grafting because the artificial dermis acts as the deep layer. Split-thickness grafts alone would not be useful where padding is required. Split grafts have a higher contracture rate than full grafts. Also, split grafts alone would not be beneficial because of the high potential for adherence. A full-thickness graft with its dermal elements would not be necessary in this case because the artificial skin provides the dermal elements. Full-thickness graft does not contract as much as split-thickness grafts. In this situation, the split graft contracture would result in a smaller, potentially more aesthetic scar.
Re-epithelialization is usually reserved for wounds measuring 1 cm or less; therefore, it would be inappropriate to not give additional treatment. Although the wound would close, the result would be less aesthetic with tendon adherence and potential dysesthesia, and it would require a longer period to heal. The reversed radial forearm flap would not be necessary and would not be long enough to reach the fingertips as well. Similarly, a radial forearm free flap would not be necessary.
2016
A 30-year-old man comes to the emergency department after falling on his outstretched left hand 6 hours ago. He injured the same hand 3 years ago and underwent open reduction and internal fixation and distal radius bone grafting to repair a metacarpal fracture of the index finger. Physical examination and x-ray study obtained today show an exposed, fractured plate. He undergoes hardware removal and multiple washouts, resulting in a 1-cm bone defect. Reconstruction of the defect is planned using bone graft from Gerdy’s tubercle of the tibia. The cortical window should be made just proximal and medial to which of the following muscles?
A) Extensor digitorum longus
B) Extensor hallucis longus
C) Peroneus longus
D) Popliteus
E) Tibialis anterior
The correct response is Option E.
The lateral tibial tubercle (Gerdy’s tubercle), on the proximal lateral tibia, is an excellent source of cancellous bone graft and would provide ample graft for use in this patient. In the patient described, the ipsilateral distal radius was harvested in the original surgery and is not available. Patient factors including obesity may make other bone graft donor sites such as the iliac crest less appealing.
Gerdy’s tubercle is located between the tibial tubercle and patellar tendon insertion to the medial side and the head of the fibula to the lateral side. Bone can be harvested through a 3- to 4-cm oblique incision, and the cortical window is made just proximal and medial to the tibialis anterior origin.
The popliteus muscle is posterior to the knee. The extensor hallucis longus and extensor digitorum longus muscles originate more distally on the tibia. The peroneus longus originates from the fibula, not the tibia.
2016
A 48-year-old man with HIV infection comes to the office requesting facial rejuvenation because of the accelerated changes he has seen since his HIV-positive status was identified. He is receiving antiretroviral therapy, has a nondetectable viral load, and normal T-cell count. Physical examination shows significant facial lipoatrophy despite the patient appearing somewhat overweight with a BMI of 27 kg/m2. The patient desires fat transfer to correct this deformity. Which of the following best describes this patient’s risk evaluation when compared with HIV-negative patients?
A) Decreased satisfaction rate
B) Higher risk of infection
C) Increased bruising
D) Increased fat graft resorption
E) Similar risk profile
The correct response is Option E.
HIV-positive patients with nondetectable viral loads and normal T-cell counts are at no higher risk for infection with transdermal procedures than HIV-negative patients. While finding adequate subdermal fat for fat harvesting can be challenging in some HIV patients because of “wasting,” or loss of fat, in patients with a normal or high BMI, fat for transfer is generally not an issue. No studies have shown higher rates of transferred fat reabsorption in HIV, while studies have shown long-term (12-month) retention using CT scans as an objective measure. Wasting is a hallmark of late-stage AIDS. Antiretroviral therapy is a mainstay of treatment for HIV-infected patients, generally improves wasting, and has dramatically improved the health and longevity of HIV-positive patients. Nonetheless, antiretrovirals are a major contributing factor to facial lipoatrophy even in stable HIV-positive patients with low or nondetectable viral loads and normal and near normal CD4 cell levels. While facial fat grafting in any patient is somewhat unpredictable, for healthy HIV-positive patients with adequate body fat, it is a reasonable approach to facial rejuvenation in patients with lipoatrophy.
Patient satisfaction and bruising should show the same variability as the HIV-negative patient.
2016
A 45-year-old man undergoes excision of a basal cell carcinoma of the mid cheek. A 3.6 × 4.7-cm oval skin defect with exposed subcutaneous fat is present. Skin grafting is planned. Which of the following is most likely to minimize long-term scar contracture?
A) Choosing a donor site with appropriate color match
B) Defatting of the skin graft
C) Harvesting with a mechanical dermatome
D) Immobilizing with negative pressure wound therapy
E) Including the entire dermis
The correct response is Option E.
The defect is a full-thickness skin defect with exposed subcutaneous fat. Coverage with a local flap and skin graft are possible reconstructive options. If skin grafting were to be performed, then a full-thickness skin graft would minimize the amount of long-term contracture (secondary contracture). A skin graft can be either split- or full-thickness. Split-thickness grafts can be harvested with a mechanical dermatome, or free hand with a scalpel. Split-thickness skin grafts do not include the entire thickness of the dermis and have less initial contracture at the time of harvest (primary contracture). Full-thickness skin grafts contain both the epidermis and the dermis and would have less long-term contracture.
Harvesting with a mechanical dermatome is useful for obtaining split-thickness skin grafts. Typical thicknesses may range from 8/1000th of an inch to 14/1000th of an inch.
Adequate immobilization of a skin graft is critical for “take” of the graft. Negative pressure wound therapy can be employed to promote adherence of the graft to the wound bed.
Defatting of the skin graft in the case of a full-thickness graft is important to optimize graft “take” in the early postoperative period.
Obtaining skin from a donor site with a close color match to the recipient site is an important aesthetic consideration, but does not affect long-term contracture.
2015
A 29-year-old woman is evaluated because of a bump that developed on the nasal dorsum 6 months after she underwent reconstruction with an onlay auricular cartilage graft to treat a post-traumatic nasal deformity. Which of the following is the most likely cause of this patient’s complication?
A) Infection
B) Ossification
C) Rejection
D) Resorption
E) Warping
The correct response is Option E.
Warping is one drawback of auricular cartilage grafts. They can curl over time. Warping is more common when the perichondrial layer is left on the graft. Pure cartilage grafts tend to warp less often. Auricular cartilage and pure cartilage warping would occur gradually over a period of weeks or months.
Cartilage is a versatile graft material that is useful for providing structural support or treating contour problems. The rib, nasal septum, and ear are the most common donor sites. Grafts are primarily composed of hyaline and elastic cartilage, with only a 1 to 10% volume of cells, so they can easily survive transplantation. Graft nutrition relies on diffusion of nutrients through the matrix of proteoglycans, interstitial fluid, and chondrocytes.
Early contour deformities could result from malposition or shifting of the graft. In this clinical case, the deformity occurs at 6 months postoperatively, when the graft should be stable in the soft-tissue envelope. Rejection is not likely with autologous cartilage and would likely occur with extrusion or fluid drainage. Rejection or failure to incorporate would typically be associated with an inadequately vascularized soft-tissue envelope or infection, and these complications would be expected within the first few weeks.
Resorption can occur gradually but is uncommon. A contour indentation would be more likely to result than a protruding bump. Ossification of the graft is not a known complication.
2015
Which of the following bone substitutes has the capacity for osteoconduction and osseointegration?
A) Hydroxyapatite
B) Polymethylmethacrylate
C) Porous polyethylene
D) Silicone
E) Titanium
The correct response is Option A.
Osteoconduction is the ability of a material to encourage bone to grow toward and along its surface. Osseointegration is defined as the direct chemical bonding of an alloplast to the surface of bone without an intervening layer of fibrous tissue. These qualities are important in identifying an appropriate bone substitute in craniofacial reconstruction.
Hydroxyapatite is a bone substitute that has capacity for both osteoconduction and osseointegration and is the base for many of most widely used bone substitutes. Hydroxyapatite is the principal mineral component of bone and comprises 60% of the calcified human skeleton. It has been used clinically for more than 25 years. It is biocompatible, and all forms are resistant to absorption after implantation.
Silicone products do not osseointegrate or osteoconduct.
Polymethylmethacrylate causes an extreme exothermic reaction associated with the setting process and is deleterious to adjacent bone and soft tissue, even with vigorous saline irrigation. It can be designed or shaped ex vivo to avoid thermal injury.
Titanium osseointegrates, but it does not osteoconduct. It provides ideal protection and reconstruction in certain clinical situations where infection is of higher concern.
High-density porous polyethylene implants have pore sizes ranging from 100 to 300 ?m. These aid in tissue ingrowth and implant fixation. These implants may be coated with polyhydroxyethylmethacrylate and calcium hydroxide. The hydrophilic nature and calcium coating result in osteoconductivity and a fibro-osseous matrix.
2015
A 40-year-old man desires correction of the appearance of his nose after traumatic injury 14 months ago. Examination shows collapse of the nasal bones and mid vault. The patient is concerned about additional scarring and donor site pain and requests a procedure with the least amount of donor site morbidity. Which of the following options is most appropriate for this patient?
A) Bone allograft
B) Costal cartilage graft
C) Iliac crest graft
D) Split calvarial graft
E) Temporal fascia graft
The correct response is Option A.
Freeze-dried bone allograft has been used extensively for orthopedic trauma and tumor reconstruction and has been demonstrated to be safe for nasal augmentation. The advantage of allograft is the avoidance of donor site harvesting and morbidity. Fresh autografts probably have more osteoinductive capacity and are likely to incorporate donor bone beds more thoroughly. Although this is important in bone grafting to injured bone, such as in a tibia fracture, it is less important in nasal grafting to a nasal soft-tissue bed. Freeze-dried allografts, much like acellular dermal grafts, are extensively processed to denture all cellular elements and therefore do not elicit immunologic rejection response. Irradiated costal cartilage allografts have also been used with success for nasal reconstruction. There is also a rare chance of disease transmission from the cadaveric donor.
Autologous costal cartilage is one of the more commonly used graft materials for nasal reconstruction, although both donor site scarring and pain are prominent. Iliac crest is a useful graft site for cortical and cancellous bone, though the shape is not ideal for nasal contouring. Donor site pain is an issue as well. The same limitations apply to split calvarial grafts, which are most useful when a bicoronal incision has already been used for craniofacial exposure.
Temporal fascia is a versatile graft source, especially when wrapped around diced cartilage. The resulting graft is pliable, soft, and has been reported to have minimal absorption. Although it is an excellent choice for this case, it does require a scalp donor site, which this patient does not want. Alloplastic materials such as silicone are also used, though they are prone to extrusion over time.
2014
An 18-year-old woman with a history of cleft lip and palate presents for secondary alveolar bone grafting. An iliac crest bone graft is planned. Which of the following characteristics of iliac crest bone graft is an advantage over the use of bone morphogenetic protein in this patient?
A) Greater volume of graft material
B) Osteoconductive properties
C) Osteoinductive properties
D) Reduced operative time
E) Reduced recovery time
The correct response is Option B.
The majority of cleft lip and cleft palate patients undergo secondary bone grafting of the alveolar cleft between the ages of 8 and 12 years. A commonly used source of graft material, iliac crest bone, is associated with morbidity including significant pain, impaired ambulation, and prolonged recovery. Some authors have proposed the use of bone morphogenetic protein for alveolar cleft closure. Advantages to this technique include reduced operative time, quicker recovery, and a greater volume of graft material, which can be limited when harvesting iliac crest bone graft in smaller children. Osteogenesis requires both osteoconductive materials and osteoinductive factors. Iliac crest bone graft displays necessary properties, while bone morphogenetic protein provides significant osteoinductive properties, but requires an additional carrier, such as demineralized bone putty, for osteoconduction. Bone morphogenetic protein is not FDA-approved for patients younger than 12 years of age.
2014
A 33-year-old woman sustains trauma to the right thigh. She undergoes debridement of the wounds. Two days later, the right anterior thigh has a 15 × 25-cm wound with areas of exposed fat and muscle. Which of the following is the most appropriate intervention to achieve wound closure?
A) Free latissimus dorsi flap
B) Full-thickness skin graft
C) Local fasciocutaneous flap
D) Negative pressure wound therapy
E) Split-thickness skin graft
The correct response is Option E.
Split-thickness skin grafts can provide wound coverage over a large area. A mechanical dermatome is often used for obtaining split-thickness skin grafts. Typical thicknesses may range from 8/1000th of an inch to 14/1000th of an inch. The graft can be meshed in various ratios such as 1:1.5, 1:2, and 1:3 to allow for a larger area of coverage per unit of harvested skin. It is important that the underlying wound bed be viable and free of necrotic tissue or infection in order to allow for healing of the skin graft (“skin graft take”). Adequate immobilization of a skin graft is important for take of the graft, and can be achieved with negative pressure wound therapy, or tie-over-bolster dressing. The thigh has an abundant amount of soft tissue and muscle, which is why skin grafts are often sufficient for wound coverage rather than flaps.
The patient has a complex wound of the anterior thigh that is best described as a degloving injury in which the skin has been sheared off of the underlying tissues. Undermining of the skin is a hallmark of this type of injury. This type of injury disrupts the blood supply to the skin and can result in tissue ischemia and necrosis. In the acute period, it can be difficult to determine the extent of tissue injury as the skin viability evolves over this time such that areas of marginal blood supply may worsen and progress to full-thickness necrosis. Before definitive wound closure can be achieved, it is critical to debride all devitalized tissue such that there is a healthy viable wound bed. Hence, performing repeat debridement is often necessary. In some cases, debriding the surrounding skin as well as the underlying fat and muscle is required to remove all necrotic tissue. Debridement should continue until healthy tissue is encountered, which can be identified by visual inspection and the presence of punctate bleeding.
The surgeon must consider several things when deciding between a flap and a graft. The reconstructive ladder may be used as a guide for management in this case. The defect is too large to achieve primary closure. The use of negative pressure wound therapy for such a large wound may be helpful as a temporary measure, but as a method of definitive wound closure would result in healing by secondary intention, scarring, and prolonged wound care. A full-thickness skin graft is not appropriate because of the large size of the defect and the amount of skin graft that would be required. A full-thickness graft would result in a major defect in another part of the body that would require primary closure. A local fasciocutaneous flap for such a large defect would require significant mobilization of tissue, and similarly, would result in a large donor site defect that would require grafting. A free flap is not necessary when there is viable soft tissue in the wound base. There is no exposed bone, tendon, nerves, blood vessels, or significant dead space, which would make a stronger argument for a flap-over-skin graft. Although not provided as an option in this question, the use of biosynthetic materials or dermal matrix tissues has been reported in the literature as an intermediate step to skin grafting, but it is important to consider the necessity of these materials in effecting outcomes in light of the significant cost of using them.
2014
A 67-year-old woman comes to the office for evaluation of abscesses on her face 5 weeks after undergoing autologous fat grafting for augmentation of the cheek. Physical examination shows multiple erythematous nodules, areas of induration, and microabscesses on both cheeks. Temperature is 99.5°F (37.5°C). Liposuction donor sites show no abnormalities. A 1-week course of ciprofloxacin prescribed by the patient’s family doctor failed to resolve the problem. Results of Gram stain and routine culture and sensitivity are negative. Which of the following is the most likely diagnosis?
A) Atypical mycobacterial infection
B) Herpes zoster infection
C) MRSA infection
D) Mucocutaneous candidiasis
E) Staphylococcus epidermidis infection
The correct response is Option A.
Mycobacteria are ubiquitous in soil and water, and infections caused by these organisms can complicate aesthetic liposuction and autologous fat-grafting procedures. The postoperative symptoms include cellulitis, abscess formation, draining sinuses, and postoperative wound infection. Patients often do not have fever, chills, or other signs of systemic infection. While patients on immunosuppressive medications seem to be at higher risk, the problem also occurs in patients with healthy immune systems. More than 50% of patients will test negative for acid-fast bacilli, in addition to negative routine culture results. Polymerase chain reaction assay testing is now available for the most common species of nontuberculous mycobacterium, and is a useful rapid screening test for patients suspected of having this diagnosis.
Bacterial infections (MRSA) would tend to show symptoms earlier, have systemic signs, and are usually easily cultured. Herpetic infections usually present with fluid-filled vesicles earlier in the postoperative course, and often have pain as a primary complaint. There is no history of previous injectable fillers, or implants, to suggest a biofilm-related infection in this patient. Mucocutaneous candidiasis is a chronic disease of the skin, nails, and mucosal surfaces.
2014
A healthy 30-year-old woman undergoes autologous fat grafting of the buttocks. The patient receives a dose of antibiotics before incision with sterile skin preparation and draping. Tumescent liposuction is performed. Gravity separation of the fat is performed intraoperatively, and 350 mL of fat is reinjected into each buttock. Postoperatively, the patient reports some areas of discrete tenderness, firmness, and limited erythema. Incision and drainage shows oily, cloudy fluid. Which of the following is the most likely cause of this patient’s complication?
A) Inadequate administration of antibiotics preoperatively
B) Inappropriate length of time for tumescent effect before aspiration
C) Lack of antibiotic administration postoperatively
D) Method of fat injection delivery
E) Use of gravity fat separation rather than centrifugation
The correct response is Option D.
The most likely cause of this patient’s complication is inadequate attention to injection delivery of microaliquots of fat, leading to fat necrosis. Liposculpting, or liposuction and fat grafting, for buttock contour improvement is increasing in popularity and becoming a frequently performed procedure. Good results can be obtained, and patient satisfaction can be high. However, complications may also occur and should not be ignored. Proper technique is an essential component of effective liposculpting. Delivery of overly large amounts of fat into inadequate substrate can lead to inadequate revascularization and fat necrosis, described in the scenario as “tenderness, firmness, and drainage of cloudy, oily fluid.” Superinfection of nonviable tissue can occur, creating “limited erythema” responsive to “a short course of oral antibiotics,” but the most likely cause is not related to preoperative or postoperative antibiotics because the patient received what can be considered appropriate antibiotic therapy for a “clean,” elective case. Neither the described 3:1 fat-to-fluid ratio nor the use of gravity fat separation is considered an inappropriate liposuction technique.
2014
A 32-year-old woman comes to the office because of capsular contracture of the right breast. She underwent bilateral augmentation mammaplasty with saline implants 9 years ago. Revision surgery using simultaneous implant exchange with fat grafting is planned. Which of the following is the most likely fat retention volume over a 6-month period in this patient?
A) 25%
B) 45%
C) 65%
D) 85%
The correct response is Option C.
Previously published work using radiologic volumetric data analysis with fat grafting for cosmetic augmentation mammaplasty demonstrates volume retention over 6 months of 64 ± 11%. Such loss of breast volume may be attributable to an element of apoptosis, a reduction in adipocyte volume after transplantation and survival, or a reduction in the fluid content of the grafted slurry. In reality, all three of these factors are likely to contribute to volume reduction over time.
2014
Cancellous bone grafts display which of the following characteristics compared with cortical bone grafts?
A) Improved osteogenic potential
B) Increased density with slower resorption
C) Increased structural support
D) Low concentrations of osteoblasts and osteocytes
E) Poor osteoinductive potential
The correct response is Option A.
Cancellous bone grafts have improved osteogenic potential when compared with cortical bone grafts. Despite significant improvements in fracture stabilization, in order to promote adequate bone union, the addition of bone grafts is occasionally necessary. These can be in the form of autografts, allografts, and synthetic bone grafts, and ortho-biologic factors. Osseous autografts can be categorized as vascularized and nonvascularized. Nonvascularized autografts can be further sub-classified as cancellous, cortical, or bone marrow aspirate. In order to choose the optimal type of graft to utilize in a specific clinical scenario, it is important to have an understanding of the properties of specific types of bone grafts as well as differences between categories of available grafts.
Bone autografts are considered the gold standard because of their immunologic compatibility as well as their osteoinductive, osteoconductive, and osteogenic healing properties. The most commonly utilized autologous bone graft is cancellous bone. When compared with cortical bone grafts, cancellous bone grafts have significant concentrations of osteoblasts and osteocytes, thus giving cancellous bone grafts superior osteogenic potential. Cortical bone grafts are dense with significant structural support, which leads to improved stability. This dense structure also leads to slower resorption compared with cancellous bone grafts, but this dense organized structure leads to lower concentrations of osteoblasts and osteocytes thus diminishing the osteogenic potential of cortical bone grafts.
2019
A 9-year-old boy is undergoing cranioplasty to repair a 5 x 5-cm congenital skull defect. Which of the following is the most appropriate material to reconstruct the cranium?
A) Costal cartilage graft
B) Cranial bone graft
C) Fibula bone graft
D) Iliac bone graft
E) Rib bone graft
The correct response is Option B.
The most appropriate material to reconstruct the cranial defect is bone graft. Autologous bone grafts are preferred for cranioplasty in the pediatric population because the material osseointegrates and grows with the child. Alloplastic implants can become dislodged as the cranium is growing and may restrict brain growth. The preferred autologous donor site for cranioplasty is the cranium because it is in the same operative field, it is associated with the lowest morbiditiy, and the graft is least likely to resorb. Cranial bone is difficult to split in younger children because a diploic space does not begin to form until approximately 5 years of age. Cranial particulate bone graft can be harvested with a bit and brace at any age because a diploic space is not required. The partial-thickness donor sites reossify and can be used again to harvest additional graft in the future. Iliac and rib donor sites are associated with significant donor site morbidity, graft resorption, and would be less ideal for reconstruction a 5 x 5 cm defect in a 9-year-old. Costal cartilage and fibula are not used as cranioplasty materials.
2019
Which of the following strategies is most effective in improving long-term viability of fat grafts?
A) Harvest fat from an abdominal donor site
B) Harvest fat with a syringe rather than a suction pump
C) Inject fat with a low-shear device
D) Process fat with telfa gauze rolling technique
E) Use tumescent solution without lidocaine
The correct response is Option C.
One of the biggest shortcomings of fat grafting is unpredictable graft survival. Fat grafting can be divided into three major steps: harvest, processing, and injection. Each step has the potential to influence the viability of transplanted fat. Fat donor site does not make a difference in fat graft viability. Lidocaine has been shown to inhibit the growth and metabolism of adipocytes. However, these effects disappear once the lidocaine is removed from the harvested fat and therefore does not affect long-term graft viability. Harvest technique, either with handheld syringe or a suction device, has not been shown to influence graft viability. Although some surgeons avoid centrifugation in an attempt to decrease trauma to fat cells, there is no objective evidence that centrifugation decreases fat cell viability. Trauma to fat cells, during processing or injection, affects fat graft survival. Injection of fat with low-shear devices has been shown to improve fat viability. Similarly, injection with larger cannulas has been shown in a few studies to increase fat survival. Strategies that hold promise in the future to increase fat cell viability include platelet-rich plasma, stem cell enrichment, and scaffolds.
2019
A 68-year-old man is diagnosed with squamous cell carcinoma of the floor of the mouth with invasion into the tongue and mandible. A radical resection with immediate reconstruction using a vascularized free fibula bone flap is planned. A vascularized bone flap is an ideal choice in this setting due to its ability to promote bony healing through which of the following pathways?
A) Endochondral ossification
B) Osteoblastic rimming
C) Osteoconduction
D) Osteogenesis
E) Osteoinduction
The correct response is Option D.
Free vascularized fibula grafts are the mainstay for mandibular reconstruction in a variety of settings, from traumatic to oncologic. Like most vascularized bone grafts, they primarily heal by osteogenesis, which involves the formation of new bone by osteoblasts from both the flap and recipient site.
In contrast, non-vascularized cortical bone grafts primarily heal by osteoconduction, or creeping substitution. In this process, the bone graft acts as a template for the ingrowth of cells and blood vessels from the recipient bed and ultimately resorbs.
Cancellous bone grafts and demineralized bone matrix heal primarily by osteoinduction. In this process, bone morphogenetic protein directly stimulates mesenchymal cells at the recipient site to differentiate into osteoprogenitor cells.
Bone fractures heal, in part, by endochondral ossification. When a bone is broken, inflammation triggers chondrocytes to form a soft callus consisting of collagen and proteoglycans at the fracture site. Through endochondral ossification, disorganized woven bone replaces the soft callus to form a hard callus which is remodeled over time into highly organized cortical bone.
Osteoblastic rimming is a histologic finding indicating the presence of bony trabeculae rimmed with osteoblasts. It is seen in a variety of bone disorders.
2019
A 55-year-old man presents with a 5 × 5-cm open wound on the medial lower leg with healthy granulation tissue. A split-thickness skin graft from the upper thigh is planned. Which of the following dressings would result in the highest degree of pain at the donor site?
A) Alginate
B) Hydrocolloid
C) Hydrofiber
D) Petrolatum gauze
E) Semipermeable
The correct response is Option D.
Petrolatum-based dressings, such as Adaptic or Xeroform, are considered nonmoist dressings. Moist dressings include semipermeable (Tegaderm or OpSite), hydrofiber (Aquacel), alginate, or hydrocolloid (DuoDERM).
In a recent meta-analysis from 2018, 41 articles with 35 prospective randomized trials found that moist dressings at a skin graft donor site are associated with less pain as compared to nonmoist dressings. When examining various time points in recovery, it was found that moist dressings showed improved pain control at every time point (postoperative days 1 to 4, 4 to 7, greater than 8).
With regard to wound healing, this finding was not universal, although most studies showed that moist dressings demonstrated improvements in re-epithelialization rate and quality of healing. Infection and cosmetic outcome were also not significantly different with variable results.
2020
A healthy 20-year-old woman presents with a deep abrasion injury of the left volar forearm that she sustained in a bicycle accident. Physical examination of the forearm shows exposed flexor tendons. The wound is debrided, and no vital nerves or vessels are exposed. The wound is approximately 4 × 4 cm. A bilaminate acellular dermal regenerative matrix is used to reconstruct the defect. The application of negative-pressure therapy is most likely to result in which of the following outcomes in this patient?
A) Increase in matrix take
B) Increase in timing to definitive skin graft
C) Negative-pressure therapy is not indicated
D) No change in matrix take
E) No change in timing to definitive skin graft
The correct response is Option A.
The application of negative-pressure therapy results in an increase in matrix take. Dermal regeneration matrix (DRM) (clinical example is Integra) is a mesh-bilayered acellular matrix composed of a cross-linked bovine tendon collagen and glycosaminoglycan dermal equivalent, and a semipermeable polysiloxane (silicone) epidermal equivalent. It is a biodegradable matrix that acts as a scaffold for fibroblast and endothelial invasion and capillary growth. DRM has been approved by the FDA (Federal Drug Administration) for use in partial- and full-thickness wounds, pressure ulcers, venous leg ulcers, surgical wounds, chronic vascular ulcers, second-degree burns, and draining wounds.
The combination of DRM with fibrin glue and postoperative negative-pressure therapy versus DRM alone in acute and chronic wounds increased the take rate from 78 to 98%. Moreover, the interval between DRM and skin transplantation was decreased from 24 to 10 days, thus decreasing the length of hospital stay (Level II evidence).
The other options are therefore incorrect. Negative-pressure therapy is commonly used in these clinical scenarios.
2020
A 20-year-old man undergoes decompressive craniectomy after a traumatic brain injury. He is now recovered from the injury. The soft tissue overlying the cranial defect is healthy and there is no communication with the paranasal sinuses. Cranioplasty with an alloplastic material is planned. A material with good osteoconductive properties is desired. Which of the following is the most appropriate choice?
A) Hydroxyapatite
B) Polyetheretherketone
C) Polymethylmethacrylate
D) Porous polyethylene
E) Titanium
The correct response is Option A.
The ideal material for cranioplasty is biocompatible, radiolucent, heat resistant, inexpensive, and has low risk for infection and extrusion. A healthy and well-perfused soft-tissue envelope is a prerequisite for alloplastic cranioplasty. Moreover, alloplasts in contact with sinuses have a high risk for infection.
Hydroxyapatite (HA) is a calcium phosphate compound with chemical structure similar to that of bone. Of the current alloplastic materials used for cranioplasty, it has the highest capacity for osteoconduction. It is available as a powder that is mixed with liquid to turn it into a malleable form that can be molded to the shape of the defect. Custom made HA ceramic implants can also be produced based on specifications of the defect. The major disadvantage of this material is that it is brittle and may fracture when stressed. It is sometimes used with a titanium mesh underlay to provide more structural stability.
Polymethylmethacrylate (PMMA) is a polymerized ester of acrylic acid. It is the most commonly used alloplastic material for cranioplasty. It is prepared in the operating room via an exothermic reaction; therefore, care has to be taken to protect the dura from thermal injury. Custom implants can also be produced. It can be easily contoured to the shape of the defect and has good mechanical strength. It does not have osteoconductive properties.
Porous polyethylene (PPE) is composed of high-density polyethylene microspheres with an interconnected porous structure. This allows tissue ingrowth in the implant. PPE is radiolucent and has been found to have an excellent safety profile. It does not have osteoconductive properties.
Polyetheretherketone (PEEK) is a semi-crystalline organic thermoplastic polymer. It is lightweight, strong, radiolucent, and heat resistant. Because of these properties, it is becoming a popular material for cranioplasty as a customized implant. It does not have osteoconductive properties.
Titanium is used as an alloy with aluminum and vanadium. It is biocompatible, non-corrosive, radiopaque, and heat resistant. Titanium mesh can be cut to the shape of the defect. It can also be used as a customized implant. The major advantages are its strength, ease of use, and low infection rate. The major disadvantage is its cost. It does not have osteoconductive properties.
2021
A 16-year-old girl requires a skin graft to the dorsal forearm after she sustained injuries in a motorcycle accident. Which of the following wound coverage techniques will lead to the LEAST secondary contraction?
A) Full-thickness skin graft, 1:4 meshed
B) Full-thickness skin graft, nonmeshed
C) Healing by secondary intention
D) Split-thickness skin graft, nonmeshed, 0.010-in thick
E) Split-thickness skin graft, nonmeshed, 0.014-in thick
The correct response is Option B.
Secondary contraction of a wound depends on various factors. Studies have shown that thicker grafts result in decreased scar depth and secondary contraction, whereas thinner grafts contract more. In terms of numbers, thick split-thickness skin grafts (0.03 in, 760 mm) approach similar final wound sizes as full-thickness skin grafts. Wider meshing results in more secondary contraction.
Myofibroblast differentiation is thought to be a key driver of contraction. Application of full-thickness skin grafts appears to speed up their life cycle, compared with wounds treated with split-thickness grafts. Conversely, thin grafts show a greater expression of alpha-smooth muscle actin, which persists for a longer time after grafting. Other mechanisms include decreased expression of pro-inflammatory genes one week after full-thickness grafting, such as insulin-like growth factor 1 (IGF1) and transforming growth factor beta-1 (TGFB1), when compared with wounds treated with thin split-thickness grafts.
Healing by secondary intention is associated with greater contraction than use of a graft.
2021
A 5-year-old girl with sarcoma of the left femur undergoes resection with a limb salvage approach including an intercalary allograft for bone reconstruction. Allografts are preferred for large segmental defects of the femur and tibia compared with cancellous bone grafts due to which of the following factors?
A) Higher mechanical strength
B) Improved osteoconduction
C) Increased graft take
D) Lower cost
The correct response is Option A.
Large defects of the femur and tibia are typically reconstructed with intercalary allografts due to their high mechanical strength. This type of reconstruction can be augmented with an intramedullary free fibula flap, which has been shown to reduce long-term complications.
Cancellous bone grafts offer superior osteogenesis, osteoinduction, and graft take in comparison with cortical grafts and allografts. Cost is not a significant consideration in reconstructing these highly complex defects. While an allograft has no donor site morbidity compared with autologous cancellous bone grafts, this is not the primary reason for their use in the described clinical scenario.
2022
A 10-year-old boy undergoes a free fibular flap reconstruction following an 8-cm resection of a chondrosarcoma on his right humerus. Which of the following best describes the primary mechanism of bone healing?
A) Endochondral ossification
B) Osteoconduction
C) Osteogenesis
D) Osteoinduction
The correct response is Option C.
Osteogenesis is the formation of new bone by osteoblasts at the host-graft interface. This is the primary mechanism by which a vascularized bone graft heals. The vascular pedicle permits the bone graft and its osteocytes to remain perfused independent of its recipient bed. Increased osteocyte survival leads to decreased bone remodeling and maintenance of bone mass and strength. Advantages of a vascularized bone graft include reconstruction of large bone defects (>6 to 8 cm) and the ability to withstand hostile recipient environments, such as irradiation and infection.
Osteoconduction (creeping substitution) is the process in which a material acts as a scaffold for bone growth, extracellular matrix, and blood vessels. Cortical bone grafts and demineralized bone matrix are examples of autogenous and exogenous osteoconductive methods.
Osteoinduction is the process of direct stimulation of mesenchymal stem cells at the recipient site by bone morphogenetic protein (BMP) to differentiate into osteoprogenitor cells. This is the primary mechanism of action for BMP and cancellous bone grafts.
Endochondral ossification is the process by which the cartilaginous soft callus covering a fracture is transformed into bone.
2022


