female reproductive system Flashcards
What does menapause begin?
- the female reproductive system remains incompletely developed until gonadotropic hormones released by anterior pituitary initiate puberty.
- the first menstrual flow begins at age 13 and repeated on a 28 day cycle throughout the womans reproductive age, except during prenancy
- menopause occurs between ages of 45-55
what age does the female reproductive developement finalize and how?
- the female reproductive system remains incompletely developed until gonadotropic hormones released by anterior pituitary initiate puberty.
- the first menstrual flow begins at age 13 and repeated on a 28 day cycle throughout the womans reproductive age, except during prenancy
- menopause occurs between ages of 45-55
Describe the tissue type and composition of the ovary cortex and medulla
- ovaries
- site of oogenesis
- histology
- almond shaped
- simple cuboidal epithelium (surface or germinal epitehlium)
- dense connective tissue capsule: tunica albuginea
-
cortex
- highly cellular (fibroblasts) connective tissue stroma
- many ovarian follicles at various stages of devopment suspended in the CT stroma
-
medulla
- contains loose connective tissue and blood vessels entering the organ through hilum from the mesenteries suspending the ovaries

What is the ovary covered by?
- ovaries
- site of oogenesis
- histology
- almond shaped
- each ovary is covered by a simple cuboidal epithelium (surface or germinal epitehlium)
- dense connective tissue capsule: tunica albuginea
- cortex
- highly cellular (fibroblasts) connective tissue stroma
- many ovarian follicles at various stages of devopment suspended in the CT stroma
- medulla
- contains loose connective tissue and blood vessels entering the organ through hilum from the mesenteries suspending the ovaries

ovaries are the stie of _______
-
ovaries
- site of oogenesis
- histology
- almond shaped
- simple cuboidal epithelium (surface or germinal epitehlium)
- dense connective tissue capsule: tunica albuginea
- cortex
- highly cellular (fibroblasts) connective tissue stroma
- many ovarian follicles at various stages of devopment suspended in the CT stroma
- medulla
- contains loose connective tissue and blood vessels entering the organ through hilum from the mesenteries suspending the ovaries

- these develope around the first month of gestation
- oogonia and primary oocytes
-
oogonia
- primoridial cells that develop after the first mont hof gestation
- these cells undergo several mitotic divisions and are found in the cortex of the developing ovary, where they continue to divide until 6th month of fetal life.
-
each ovary posses ~3million oogonia, but most undergo atresia
- process of degeneration and death
- primary oocyte
- result from the final mitotic division of the surviving oogonia
- begin meiosis while still in the fetus, but are arrested in prophase of first meitotic division
- remain arrested in this stage until just before ovulation
- young woman has ~400000 follicles, when ovulation begins around puberty
-
oogonia
- quick math
- ovary starts with 300million oogonia
- 400k are arrested in P1 as follicles in a young woman who starts puberty
- only 500 oocytes are ovulated over a lifetime
- meaning that 99% of the oocytes undergo atresia
- results from the final mitotic division of the surviving oogonia. Describe the process leading up through meiosis
- oogonia and primary oocytes
- oogonia
- primoridial cells that develop after the first mont hof gestation
- these cells undergo several mitotic divisions and are found in the cortex of the developing ovary, where they continue to divide until 6th month of fetal life.
- each ovary posses ~3million oogonia, but most undergo atresia
- process of degeneration and death
-
primary oocyte
- result from the final mitotic division of the surviving oogonia
- begin meiosis while still in the fetus, but are arrested in prophase of first meitotic division
- remain arrested in this stage until just before ovulation
- young woman has ~400000 follicles, when ovulation begins around puberty
- oogonia
- quick math
- ovary starts with 300million oogonia
- 400k are arrested in P1 as follicles in a young woman who starts puberty
- only 500 oocytes are ovulated over a lifetime
- meaning that 99% of the oocytes undergo atresia
discuss and label all 5 major steps in follicular development
- ovarian follicles
-
primordial follicles
- most primitive follicles
- each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
- primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
-
primary follicles unilaminar
- develop from the primordial follicle
- surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
- a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
-
multilaminar primary follicle
- a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
- formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
- composed of
- glyocproteins secreted by both follicular cells and the oocyte
- theca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
- orgaizes into 2 distint layers
- theca interna
- form from the connective tissue immediatly surrounding the basal lamina
- theca externa
- the conncective tissue layer surrounding the theca interna
- theca interna
- a primary follicle with 2 or more layer of granulosa cells
-
secondary follicle( antral follicle)
- increase in granulosa cell population, from FSH leads to
- cumulus oophus
- group of granulosa cells associated with the oocyte
- corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
- cumulus oophus
- increase in granulosa cell population, from FSH leads to
-
graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus anflota freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
-
primordial follicles

a follicle is found wit ha single layer of squamous follicular cells.
- What is the stage
- what is the location?
- describe the attachment and seperation of them
- ovarian follicles
-
primordial follicles
- most primitive follicles
-
each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
-
primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
- primary follicles unilaminar
- develop from the primordial follicle
- surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
- a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
- multilaminar primary follicle
- a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
- formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
- composed of
- glyocproteins secreted by both follicular cells and the oocyte
- tehca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
- orgaizes into 2 distint layers
- theca interna
- form from the connective tissue immediatly surrounding the basal lamina
- theca externa
- the conncective tissue layer surrounding the theca interna
- theca interna
- a primary follicle with 2 or more layer of granulosa cells
- secondary follicle( antral follicle)
- increase in granulosa cell population, from FSH leads to
- cumulus oophus
- group of granulosa cells associated with the oocyte
- corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
- cumulus oophus
- increase in granulosa cell population, from FSH leads to
- graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus anflota freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
-
primordial follicles

a follicular cell is surrounded by a single layer of cuboidal follicular cells
- what is the stage
- ovarian follicles
- primordial follicles
- most primitive follicles
- each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
- primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
-
primary follicles unilaminar
- develop from the primordial follicle
-
surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
-
a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
- multilaminar primary follicle
- a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
- formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
- composed of
- glyocproteins secreted by both follicular cells and the oocyte
- tehca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
- orgaizes into 2 distint layers
- theca interna
- form from the connective tissue immediatly surrounding the basal lamina
- theca externa
- the conncective tissue layer surrounding the theca interna
- theca interna
- a primary follicle with 2 or more layer of granulosa cells
- secondary follicle( antral follicle)
- increase in granulosa cell population, from FSH leads to
- cumulus oophus
- group of granulosa cells associated with the oocyte
- corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
- cumulus oophus
- increase in granulosa cell population, from FSH leads to
- graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus anflota freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
- primordial follicles

a follicle is surrounded by a zona pellucida and several layers of granulosa cells
- what atage is it in?
- describe the other structures associated with this stage and the physiology
- ovarian follicles
- primordial follicles
- most primitive follicles
- each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
- primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
- primary follicles unilaminar
- develop from the primordial follicle
- surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
- a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
-
multilaminar primary follicle
-
a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
-
formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
-
composed of
- glyocproteins secreted by both follicular cells and the oocyte
-
theca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
-
orgaizes into 2 distint layers
-
theca interna
- form from the connective tissue immediatly surrounding the basal lamina
-
theca externa
- the conncective tissue layer surrounding the theca interna
-
theca interna
-
a primary follicle with 2 or more layer of granulosa cells
- secondary follicle( antral follicle)
- increase in granulosa cell population, from FSH leads to
- cumulus oophus
- group of granulosa cells associated with the oocyte
- corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
- cumulus oophus
- increase in granulosa cell population, from FSH leads to
- graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus anflota freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
- primordial follicles

a follicle has generated a cumulous oophus.
- what stage is it in?
- what other structure are present?
- list their function
- ovarian follicles
- primordial follicles
- most primitive follicles
- each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
- primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
- primary follicles unilaminar
- develop from the primordial follicle
- surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
- a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
- multilaminar primary follicle
- a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
- formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
- composed of
- glyocproteins secreted by both follicular cells and the oocyte
- tehca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
- orgaizes into 2 distint layers
- theca interna
- form from the connective tissue immediatly surrounding the basal lamina
- theca externa
- the conncective tissue layer surrounding the theca interna
- theca interna
- a primary follicle with 2 or more layer of granulosa cells
-
secondary follicle( antral follicle)
-
increase in granulosa cell population, from FSH leads to
-
cumulus oophus
- group of granulosa cells associated with the oocyte
-
corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
-
cumulus oophus
-
increase in granulosa cell population, from FSH leads to
- graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus anflota freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
- primordial follicles

the primary oocyte is found floating in the middle of the antrum.
- what stage is it in?
- what other structures are present?
- list their functions
- ovarian follicles
- primordial follicles
- most primitive follicles
- each consists of
- primary oocyte surrounded by a singla layer of squamous follicular cells
- the oocyte is 25micrometes in diameter at this stage, the follicular cells are attached to one another by sedmosomes and havea basal lamina seperating the follicle from surrounding stromal connective tissue
- primordial follicles location
- found adjacent to the tunica albuginea in the mature ovary
- primary follicles unilaminar
- develop from the primordial follicle
- surrounding cell maturation
- the follicular cells surrounding the primary oocyte become cuboidal in shape
- a primary follicle is surrounding by a. single layer of cuboidal cells
- the primary oocyte grows to 100-150 micrometers, developing a large nucleus
- multilaminar primary follicle
- a primary follicle with 2 or more layer of granulosa cells
- granulosa cells function to assist flow of nutrients and other molecules between the blood and follicular fluid
- formation of the zona pellucida
- distinct acidphilic refractile layer develops between oocyte and the follicular calls
- composed of
- glyocproteins secreted by both follicular cells and the oocyte
- tehca folliculi
- organized layer of connective tissue outside of the basal lamina of the primary follicle
- orgaizes into 2 distint layers
- theca interna
- form from the connective tissue immediatly surrounding the basal lamina
- theca externa
- the conncective tissue layer surrounding the theca interna
- theca interna
- a primary follicle with 2 or more layer of granulosa cells
- secondary follicle( antral follicle)
- increase in granulosa cell population, from FSH leads to
- cumulus oophus
- group of granulosa cells associated with the oocyte
- corona radiadata
- lies immediatly outside the zona pellucida
- first single layer of granulosa cells surrounding the oocyte
- remains with oocyte at the time of oculation, unlike other granulosa cells
- cumulus oophus
- increase in granulosa cell population, from FSH leads to
-
graafian follicle (mature follicle)
- granulosa cell proliferation and liquor folliculi accumulation continues unti mature graafian follicle is formed
- 2/5cm
- priamry ooctye + cornoa radiata detach from the cumulus oophorus and float freely in liquor folliculi
- theca interna is more pronounced
- this is when the secondary oocyte is formed
- primordial follicles

describe the meisosis events in the generation of a corpus luteum. Be location and stage specific
formation of the secondary oocyte in the graafian follicle
-
secondary oocyte
-
forms when the primary oocyte in the graafian follicle compeltes the first meitotic division
- remember all the oogonium are arrested in Prophase1 in the begining of the life cycle for females
- secondary oocyte enters the second meitotic division and is arrested in metaphase
- after being arrested in M2
- the secondary oocyte is oculated WITH THE CORONA RADIATA
- the remnants of the graafian follicle generate a corpus luteum
-
forms when the primary oocyte in the graafian follicle compeltes the first meitotic division

a oocyte is found is taken up for collection in the uterine tube
- Was meiosis complete? assume no sexual history
- what does the graafian follicle become?
formation of the secondary oocyte in the graafian follicle
-
secondary oocyte
-
forms when the primary oocyte in the graafian follicle compeltes the first meitotic division
- remember all the oogonium are arrested in Prophase1 in the begining of the life cycle for females
- secondary oocyte enters the second meitotic division and is arrested in metaphase
-
after being arrested in M2
- the secondary oocyte is oculated WITH THE CORONA RADIATA
- the remnants of the graafian follicle generate a corpus luteum
-
forms when the primary oocyte in the graafian follicle compeltes the first meitotic division

what type of oocyte is ejected from the ovary and with what structure?
formation of the secondary oocyte in the graafian follicle
- secondary oocyte
- forms when the primary oocyte in the graafian follicle compeltes the first meitotic division
- remember all the oogonium are arrested in Prophase1 in the begining of the life cycle for females
- secondary oocyte enters the second meitotic division and is arrested in metaphase
- after being arrested in M2
- the secondary oocyte is oculated WITH THE CORONA RADIATA
- the remnants of the graafian follicle generate a corpus luteum
- forms when the primary oocyte in the graafian follicle compeltes the first meitotic division

what occurs during ovulation, theoretically is occurs how often?
ovulation
- the release of oocyte from the ovary, occurring at ~14th day of the 28 day menstrual cycle
- oculation is a result of several homronally induced factors
- increased volume and pressure of liquor folliculi
- enzymatic breakdown of the follicular wall
- contraction of smooth muscle in the theca externa
- stigma
- area on the ovary surface that becomes ischemic dur to the pressure of the Graafian follicle against the ovarian wall
- the tissue bvecomes necrotic and ruptures ( along with the follicular wall)
- the oocyte is released through this opening and is transported into the oviduct.

what notable changes results in ovulation
ovulation
- the release of oocyte from the ovary, occurring at ~14th day of the 28 day menstrual cycle
-
ovulation is a result of several homronally induced factors
- increased volume and pressure of liquor folliculi
- enzymatic breakdown of the follicular wall
- contraction of smooth muscle in the theca externa
-
stigma
- area on the ovary surface that becomes ischemic dur to the pressure of the Graafian follicle against the ovarian wall
- the tissue bvecomes necrotic and ruptures ( along with the follicular wall)
- the oocyte is released through this opening and is transported into the oviduct.

area on the ovary surface tha becomes ischemic due to pressure of the graafian follicle. what happens to this area?
ovulation
- the release of oocyte from the ovary, occurring at ~14th day of the 28 day menstrual cycle
- oculation is a result of several homronally induced factors
- increased volume and pressure of liquor folliculi
- enzymatic breakdown of the follicular wall
- contraction of smooth muscle in the theca externa
-
stigma
- area on the ovary surface that becomes ischemic dur to the pressure of the Graafian follicle against the ovarian wall
- the tissue bvecomes necrotic and ruptures ( along with the follicular wall)
- the oocyte is released through this opening and is transported into the oviduct.

during ovulation
- what increases in volume?
- how does the follicular wall break down?
- Where does smooth muscle contraction occur?
- what occurs in the stigma?
ovulation
- the release of oocyte from the ovary, occurring at ~14th day of the 28 day menstrual cycle
-
oculation is a result of several homronally induced factors
- increased volume and pressure of liquor folliculi
- enzymatic breakdown of the follicular wall
- contraction of smooth muscle in the theca externa
-
stigma
- area on the ovary surface that becomes ischemic dur to the pressure of the Graafian follicle against the ovarian wall
- the tissue bvecomes necrotic and ruptures ( along with the follicular wall)
- the oocyte is released through this opening and is transported into the oviduct.

forms from the remnants of collapsed graafian follicle.
- describe the cell types and products
-
corpus luteum
- formed from the remnants of collapsed graafian follicle after oculation
- a blood clot is formed at the rupture site and the modified granulosa and theca interna cells begin secretion of veious hormones
-
granulosa lutein cells
- ~80 of structure
-
synthesis steroid and highly dense with the cellular machinary to synthesize cholesterol and downstream products
- estrogen
- progesterone
-
theca lutein cells
- small dark staining cells derived from the theca interna
-
synthesize
- progesterone
- androgens
- degenerate 14 post ovulation if fertilization does not occur
- corpus albicans
- dense connective tissue scar formed at the site of an involueted corpus luteum

dense connective tissue sxar formed at the site of an involuted corpus luteum
- corpus luteum
- formed from the remnants of collapsed graafian follicle after oculation
- a blood clot is formed at the rupture site and the modified granulosa and theca interna cells begin secretion of veious hormones
- granulosa lutein cells
- ~80 of structure
- synthesis steroid and highly dense with the cellular machinary to synthesize cholesterol and downstream products
- estrogen
- progesterone
- theca lutein cells
- small dark staining cells derived from the theca interna
- synthesize
- progesterone
- androgens
- degenerate 14 post ovulation if fertilization does not occur
-
corpus albicans
- dense connective tissue scar formed at the site of an involuted corpus luteum

describe the following with regard to the corpus luteum
- synthesize estrogen and progesterone, ~80% of the cells in the corpus luteum
- small dark, staining cells synthesize: progesteron and androgens
- what occurs in these cells 14 days after ovulation
- corpus luteum
- formed from the remnants of collapsed graafian follicle after oculation
- a blood clot is formed at the rupture site and the modified granulosa and theca interna cells begin secretion of veious hormones
-
granulosa lutein cells
- ~80 of structure
-
synthesis steroid and highly dense with the cellular machinary to synthesize cholesterol and downstream products
- estrogen
- progesterone
-
theca lutein cells
- small dark staining cells derived from the theca interna
-
synthesize
- progesterone
- androgens
- degenerate 14 post ovulation if fertilization does not occur
- corpus albicans
- dense connective tissue scar formed at the site of an involuted corpus luteum
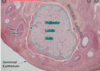
what are the hormones that control the follicle development and ovulation? (3 main ones)
hormonal control of follicle development and ovulation is largely dependent on FSH and LH
-
FSH
- the most influential hormone in the days 8-10 of mentrual cycle
- stimulates 10-20 primary follicles to develop
- origin
- released from pituitary pars distalis
- binds to receptors on the follicular cell surface
- cells enlarge and proliferate in response to FSH stimulation, formining the layers of granulosa cells in the multilaminar primary follicle.
- granluosa cells induce production of estrogen leading to secondary follicle development
-
LH
- sythesis and release
- pars distalis
- stimulated by increased estrogen
- occurs around day 14
- sharp increase in LH release results from high circulating levels of estrogens
- binds to receptors on the theca interna cells
- stimulated production of androgens
- Androgen produced by the theca interna is converted to estrogen by the granulosa cells
- rising estrogen levels suppresses FSH release from pars distalis
- directly on the anterior pituitary
- and indirectly on the hypothalmus, decreasing GnRH
- function
- induces the primary oocyte to complete meiosis 1 and proceed to metaphase 2
- high levels also induce ovulation
- post ovulation the corpus luteum is formed and maintained dur to binding of LH to receptors on theca interna
- sythesis and release
-
progesterone
- synthesized in both cell lines
- theca lutein
- granulosa cells
- function
- inhibits release of LH
- directly on the anterior pituitary
- indirectly, via on the hypothalmus to decrease the GnRH
- inhibits release of LH
- fertilization?
- no
- LH levels fall below levels required to maintain corpus luteum and it will consequently begin to degenerate
- occurs ~14days post ovulation
- no
- synthesized in both cell lines




























