1 - Hypersensitivity Reactions and Diseases Flashcards
What is the main cause of immunodeficiency in the UK?
Malnutrition in the elderly

Give some examples of autoimmune conditions.
Disease or systemic specific

What is the definition of hypersensitivity?
- Antigen-specific immune responses that are either inappropriate or excessive and result in harm to host by damaging tissue or changing a tissues function
- Mechanisms are the same as the normal immune response

What are the two categories of triggers for hypersensitivity?
- Exogenous antigens:
- Non infectious substances (pollen, dust)
- Infectious microbes (sepsis)
- Drugs (penicillin)
- Intrinsic anigens:
- Infectious microbes (mimicry like rheumatic fever)
- Self antigens (auto-immunity)

What are the different types of hypersensitivity reactions?
- Type I / immediate (Allergy)
- Type II / antiBody mediated
- Type III / immune Complexes mediated
- Type IV / cell mediated (Delayed)
- First 3 are antibody mediated, but 4 has antibody but not primary cause

What are the two phases of hypersensitivity reactions?
Sensitisation:
- First encounter with antigen
- Activation of APCs and memory effector cells
- A previously exposed individual to the antigen is said to be “sensitized”
Effector:
- Reaction upon reexposure to the same antigen and activation of the memory cells of the adaptive immunity

Which antigens are involved in Type I hypersensitivity?
Environmental non-infectious antigens
How long does it take for a type II hypersensitivity reaction to be triggered, what antibodies are involved and what antigens are targeted?
- 5-12 hours
- IgG or IgM
- Causes tissue damage or physiological change
- Targets cell bound antigens so organ specific:
- Exogenous: blood group antigens, rhesus D antigens
- Endogenous: self antigens
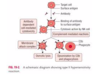
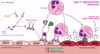
What are the mechanisms in type II hypersensitivity that lead to cell/tissue damage?
- Complement activation: cell lysis (MC), neutrophil recruitment/activation (C3A/C5A), opsonisation (C3b)
- Antibody-dependent cell cytotoxicity: NK cells
- Antibody binds to antigen and activates complement

What are some examples of diseases caused by a type II hypersensitivity reaction?

What is the mechanism behind haemolytic transfusion reactions?
- Type II hypersensitivity IgM
- Incompatability in ABO or rhesus D antigens
- Donor RBC destroyed by recipients immune system through IgM
- Caues shock, kidney failure, circulatory collapse and death

What is the mechanism behind haemolytic disease of the newborn?
Type II hypersensitivity reaction IgG
- Involves Rhesus D antigen
- Mismatch between mother(Rh-) and child (Rh+) and thus antibodies are produced against Rh+ antigen
- After 2nd pregnancy, IgG antibodies cross placenta and cause HDN

How can we prevent haemolytic disease of the newborn?
When mother is Rh -ve she is given RhoGAM within 3 days of miscarriage or delivery of Rh +ve infant to bind all of the Rhesus antibodies

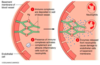
What mechanisms in a type II hypersensitivity reaction lead to physiological changes and give two examples of disease caused by this?
- Antibody can stimulate or block a receptor

What therapeutic approaches can be used to combat tissue/cell damage and physiological change induced by type II hypersensitivity reactions?
- Immune suppression for complement activation
- Plasmapheresis for circulating antibodies and inflammatory mediators
- Splenectomy for opsonisation/Phagocytosis
- Intravenous immunoglobulin (IVIG) for IgG degradation and hopefully bad IgG will degrade
(see image for physiological change)

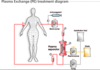
What is plasmapheresis therapy and what diseases is it used for?
- Removal of antibodies from the plasma allowing short term relief and healing of damaged tissue
- Used in myasthenia gravis, goodpasture’s syndrome and grave’s as these all are primary antibodies that drive the disease